Cataracts
This guide will help you learn more about:
- how cataracts develop
- how cataracts are treated with surgery
- what kind of costs to expect, and
- how long it will take you to recover from surgery
The information will help you be more educated and involved in your eye doctor’s treatment through diagnosis, surgery and recovery.


What is a Cataract?
A cataract is a clouding of the eye’s lens, which blocks or changes the passage of light into the eye. The lens of the eye is located behind the pupil and the colored iris, and is normally transparent. The lens helps to focus images onto the retina – which transmits the images to the brain.
Your vision may become blurry or dim because the cataract stops light from properly passing through to your retina.
How common are cataracts?
Cataracts are a leading cause of blindness among older adults in the United States. More than half of all Americans have cataracts by the time they are 80 years old. Cataracts can also sometimes be found in young people or even newborn babies.
Am I at risk for developing cataracts?
The exact cause of a cataract is unknown. Most often, a cataract is part of getting older. As you age, you are at greater risk of developing a cataract. There are also several possible risk factors for cataracts, such as:
- Intense heat or long-term exposure to UV rays from the sun
- Certain diseases, such as diabetes
- Inflammation in the eye
- Hereditary influences
- Events before birth, such as German measles in the mother
- Long-term steroid use
- Eye injuries
- Eye diseases
- Smoking
What are the symptoms of a cataract?
Generally, a cataract does not cause pain, redness or tears. The following problems may indicate that you have a cataract:
- You have blurred vision, double vision, ghost images, or the sense of a “film” over your eyes.
- Lights seem too dim for reading or close-up work, or you are “dazzled” by strong light.
- You change eyeglass prescriptions often and the change does not seem to help your vision.
- You may also be able to see the cataract in your eye. It may look like a milky or yellowish spot in your pupil.
Why do cataracts form?
Cataracts are probably caused by changes related to aging. Throughout our lives, our bodies replace old cells with new ones. As we grow older, the old cells in our eye’s lens build up and block light as it tries to pass through. The end result is cloudy vision.
Besides getting older, other factors may cause cataracts to form. Eye infections, some medicines (such as steroids), injuries or exposure to intense heat or radiation may cause cataracts. Too much exposure to non-visible sunlight (called UV or ultraviolet light) and various diseases, such as diabetes or metabolic disorders, may also contribute to cataracts forming.
What are the types of cataracts?
Age-related – 95% of cataracts are age-related, usually after age 40.
Congenital – These are present at birth, usually caused by infection or inflammation during pregnancy; possibly inherited.
Traumatic – Lens damage from a hard blow, cut, puncture, intense heat or chemical burn may cause cataracts.
Secondary – Some medicines, eye disease, eye infection, or diseases such as diabetes cause these cataracts.
Cataracts usually form in both eyes, but not at the same rate. They can develop slowly or quickly, or progress to a certain point, then not get any worse. As a result, you may not notice large changes in your sight right away.
How will my eye doctor check for cataracts?
Everyone who gets a cataract experiences it differently. But a person with a cataract commonly experiences cloudy or blurry vision. Lights may cause a glare, seem too dim or seem too bright. It may be hard to read or drive, especially at night. If you have a cataract, you may see halos around lights, such as car headlights, that make it hard to focus clearly. Colors may not seem as bright as they used to be. Or you may have to change your eyeglass prescription often.
If you notice any of these changes, make an appointment to see your eye doctor.
If you have a cataract, you may have symptoms that are similar to those of other eye diseases. Only your eye doctor can tell you for sure what’s wrong.
To find out if you have cataracts, your eye doctor will want to:
- find out your general medical history
- find out your specific eye history, including problems and symptoms
- test your vision (visual acuity)
- test your side vision (peripheral vision)
- test your eye movement
- test you for glaucoma (by measuring the eye’s internal pressure)
- do a microscopic exam of the front of the eye (using something called a slit lamp) to assess the density of the cataract and how it interferes with light passing through the lens
- widen (dilate) the pupils of your eyes to examine the retina, the optic nerve (which carries visual messages from the retina to the brain) and the macula (responsible for the best part of central vision)
- test you to see how glare affects your vision
After this exam, your eye doctor will determine whether you have cataracts, how much they interfere with your vision, whether surgery would help, and what types of treatment and lens replacements are best for you.
Cataracts and Vision Loss
Your eye works like a camera. A camera needs a lens to focus an image. But when the lens is dirty or cloudy, the camera can’t take a good, clear picture.
It’s the same with your eyes. Your eye lens focuses rays of light on the nerve tissue at the back of your eye (the retina). The retina then transmits a clear image to your brain. But when a cataract clouds your eye’s lens, light rays don’t pass through as well and the retina cannot transmit a good picture.
About one in six Americans age 40 and older will get a cataract. By age 80, more than half will have a cataract. Because everyone is different, some people may not notice a large change in their eyesight. Others will find it a challenge to enjoy even the simplest tasks and may find it harder and harder to stay independent.
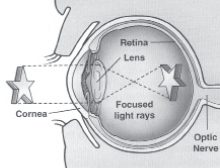
Light passes through a normal eye
without anything blocking its way.
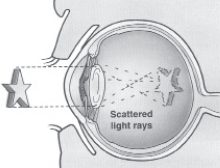
When the lens of your eye becomes cloudy,
the cataract prevents you from seeing clearly
by preventing enough light from passing through.
Cataract Surgery
Cataract surgery has restored vision to millions of people. Every year in the U.S., more than two million cataract surgeries are performed.
The key to preventing vision loss is regular eye exams. If you are 65 or older, you should get a complete eye exam every one or two years, even if you have no problem seeing well. Be sure to ask your eye doctor for a dilated eye exam.
Every year in the U.S., more than two million cataract surgeries are performed. Cataract surgeries are performed without complication in over 95% of cases. Still, you will likely have questions, fears or reservations about the procedure.
